The good old National Health Service. Even the Tories can not be seen to openly attack the principle of health care free at the point of delivery for all (despite the fact that Jeremy Hunt, the current Secretary for Health co-authored a book calling for the NHS to be replaced by an insurance based American kind of system in 2005.) The recent struggles the government had trying to impose a different contract on NHS doctors has also forced the Tories onto the back foot- never underestimate the power wielded by the medical profession. It could be argued that there are some other subtle political battles being played out in the media however- despite the massive success of the NHS in just about every international league table, every story you read in the papers is negative.
What gets far less media attention however is something that our health system depends on entirely, so much so that we have been attempting to formally integrate for at least 30 years- I refer of course to the social care system.
I know about this stuff- I have worked in the system for years. I wanted to write something that described the reality of what the system is like so began typing this…
By any measure, social care systems in the UK are in crisis (and I do not use the ‘c’ word lightly.) Check out this from The Observer the other day;
Data from 98 of the 151 local authorities in England with statutory responsibility for social care show that they met only 218 (42%) of 515 targets to improve social care in their area and missed the other 297 (58%).
Under the Better Care Fund councils receive money, mainly from the NHS budget, in return for introducing schemes to reduce demand for hospital care. This is done, for example, by providing better care for people in their own home or in care homes. But the FoI responses reveal that councils met barely a quarter of their targets in 2015-16 for reducing non-elective (emergency) admissions to hospital…
…“Just at the point when the NHS desperately needs more out of hospital care, we seem to be going backwards in many places. That can’t be right,” Hopson said.
Stephen Dalton, chief executive of the NHS Confederation, said: “These figures are very worrying as we head into what could be a very tough winter for the NHS. We only need a significant dip in the weather, which has been mild so far, and people would become more vulnerable and we would see a big spike in demand. We have a perfect storm going on at the moment of unprecedented demand for care, the fact that we have reached a tipping point in terms of the demographics, and cuts to local councils that are among the biggest in their history.”
Leave aside the fact that not even The Observer seems to be able to find someone who works in social care to comment, the picture seems to be pretty bleak. We have an aging population, not only because of a population bulge that is maturing at the same time, but also because people are living much longer. The longer people live, the more likely they are to have health problems that require care and support, particularly people who develop some form of dementia.
The response from our health and social care system has been to increasingly care for people in their own homes. In general it is possible to argue that this is a good thing, but it is also much cheaper, allowing expensive in-patient and total care resources to be targeted at those in the most need. It requires effective and efficient co-ordination between hospital staff and community based care staff, who traditionally have different employers and work to totally different agendas.
My work experience over the last 15 years has been in Scotland, where the government has now required all health and social care services to become fully integrated, sharing a management and funding system- this has been far from a straightforward and integration looks very different in different part of the country. However in theory some of the boundaries and complex funding regimes have been simplified.
What is really going on then? Reflecting on my own experience, here is my list of what seems to be creating the problem;
Money
There is not much of it around. Social Care is funded by Local Authorities. The scale of cuts to local authorities is staggering- when you have (allegedly) secret deals between government and flagship Conservative councils to avoid them holding a crisis referendum, you know things are bad. Most Local Authorities have now faced year on year cuts to allocation of funding from central government. What happens is that most authorities will use ‘reserves’ to give them some breathings space and then a process of identifying savings will begin- typically along these lines;
- Wages will be frozen, so that staff will not get any kind of inflation uplift
- Vacant posts will not be filled
- ‘non essential’ services will be targeted first- this includes all sorts of things that are precious to some- lunch clubs, libraries, sports facilities, public toilets, grass verge cutting etc. These cuts will often have unexpected consequences, in that a cut to one service increases costs to others.
- ‘External’ funding, to voluntary groups, third sector organisations, even when these provide essential contracted services, will be hit hardest- this is always easier for councils as they export the pain of having to make the savings.
- This will not be enough however, so councils will have to make staff redundant. They will start by asking staff to make themselves ‘voluntarily’ redundant- but this can be expensive, as typically those who will want to go are older, with more years of service.
- Councils will have to raise Council Tax. The Government lifted the freeze, and most councils will have no choice. This is clearly a political game- preferable to a raise in income taxes.
If you want to know more about the projections of costs over the next few years- have a look at this document.
Change in actual provision of services
As well as the cuts above, increasingly key services that have been provided by Local Authority staff will be ‘outsourced’ to third sector organisations and businesses. This will be done primarily in order to drive down costs, but also because of a rhetoric around efficiency and change management. This in itself is not necessarily a bad thing- but brings a totally different landscape of service provision, particularly within social care.
Typically, the way services are commissioned within LAs has two main areas of development;
Firstly there is the identification of providers in an area- home care organisations for older people, specialist support for people with LD, Mental Health problems, children with special needs etc, care homes, nursing homes. Increasingly LA’s are not providing these services directly at all- they are entirely reliant on establishing and maintaining a local ‘marketplace’ of providers. They may do this by ‘tendering’ for specific block contracts, but these have to be commercially attractive and increasingly the margins are so small that many providers regard their businesses as no longer viable.
When you consider what social care providers have to undertake, the marginality of their survival is obvious. They operate in a highly regulated environment, with scrutiny from both independent regulators and Local Authority commissioning processes. They provide services in some of the most challenging and difficult circumstances, but because of the squeeze downwards of costs, are only able to pay very low wages (often minimum wage, with zero hour contracts) and provide minimum training.
Maintaining the ‘market place’ in a context of dwindling finances is a major challenge. IN some area of the country there are major gaps. This is particularly noticeable in nursing home provision.
Secondly, there is the commissioning process for individuals. This typically starts by an ‘assessment’ by a social worker or nurse, who will identify what specific needs an individual has and put together a ‘care plan’. This kicks off what can then be a bewildering bureaucratic process, involving the calculation of an ‘indicative budget’, often through the use of complicated formulas that make assumptions about contributions based on income. Some care will be free, other care will be chargeable. Also in Scotland the ‘Self Directed Care’ process will have to be discussed, giving people the right to commission their own services, using the indicative budget.
Remember that all this process is taking place at the point when most those in need of services are at their most vulnerable and potentially least able to provide necessary information. Most LAs have the ability to provide some emergency care, pending the completion of the bureaucracy, but this does not typically apply when someone is in hospital.
When I began my career in social work, most services were provided directly by LAs. If you needed a service, you sent a referral form. You checked the care was working by holding a review at six weeks then six months. The process is wholly different now- in some ways things are much better- there is much more choice and autonomy for those who are able enough to make use of it. There is a greater variety of kinds of care. Care is more typically at home.
At the same time however, getting the service you need remains to some degree a lottery- where you live in the country, how good you are at understanding your rights, how good your social worker is at manipulating the system in your favour. Navigating the complex bureaucracy is rarely straightforward and it is not surprise that things can go wrong- leading to delays and great stress for all involved.
Demographics
As well as having to cope with lower funding, LAs also have rising cost pressures, not least because of an increasing population of older people. This increase is in part a feature of the ageing of ‘Baby Boomers’, but also because people are living longer. The older we are the more likely we are to have health and care issues such as dementia. As well as in increase in people over 70, there has also been an increase in those over 80, over 90, over 100.
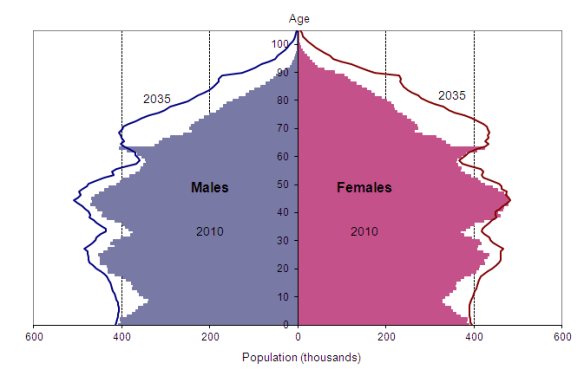
(Image and more detail here)
Clearly this imposes a huge challenge on services. incidentally, this is one of the reasons why we need immigrants in this country- they tend to be younger, have higher birth rates, and their productivity has good impact on the economy.
It also means that people who have much greater needs (eg people who are bedbound, or people who need 24 hour supervision because of challenging dementia) are increasingly care for at home, with a mixture of home care type services and electronic aids. When things go wrong with these packages of care – as they are bound to for things like deterioration in illness, breakdown through carer stress, etc. – then the only fall back tends to be admission to hospital.
In summary, Health Services do not operate in isolation. Increasingly they depend on a range of social care and community care services. Governments, for political reasons, have sought to defend core funding for the NHS, but have at the same time made cuts that continue to devastate social care. Unsurprisingly this has had a direct impact on NHS inpatient services, leading to the crisis that fills our newspaper.
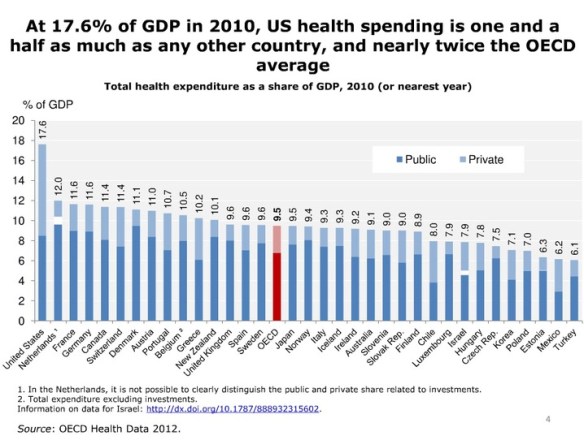
One more point to make- we are being told that we ‘can not afford’ the services that we have been used to. Accepting that money may not always be the answer, it might be interesting to note the percentage of our GDP that we spend on health care in this country as opposed to other Western democracies. We are very much ‘mid table’.